Lipedema
A condition that causes excess fat to accumulate in the lower part of the body, leading to heavy and painful legs.
Lipedema is a chronic fat distribution disorder that causes symmetrical enlargement of the legs, tenderness, easy bruising, and resistance to weight loss. It is frequently underdiagnosed and confused with obesity or lymphoedema.
Book a Consultation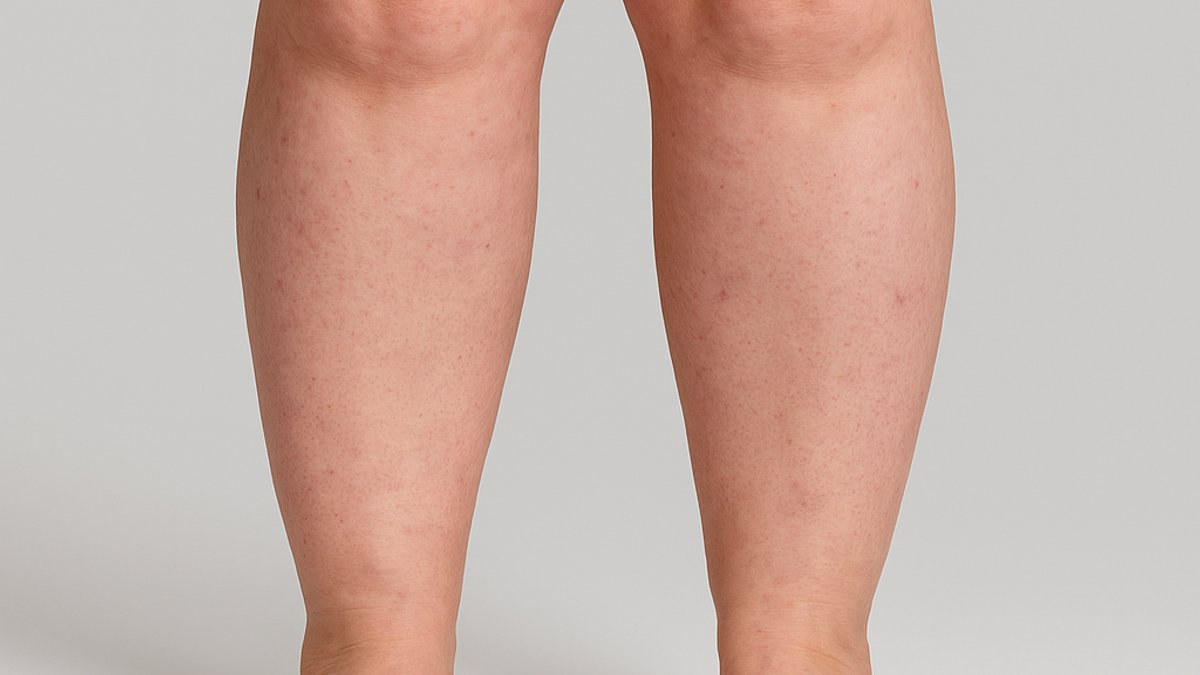
Lipedema is often misdiagnosed as standard weight gain, but it is a distinct condition that causes painful, symmetrical fat accumulation in the limbs.
Symptoms
- Bilateral, symmetrical leg enlargement from hips to ankles (feet typically spared)
- Soft, tender tissue that bruises easily with minor trauma
- Heaviness, aching, and leg fatigue worsening throughout the day
- Resistance to weight loss through diet or exercise alone
Stages of Lipedema
- Stage 1 — smooth skin with early subcutaneous fat enlargement
- Stage 2 — skin dimpling and nodular texture
- Stage 3 — pronounced column-like deformity with larger skin folds
- Stage 4 (Lipo-lymphoedema) — secondary lymphatic dysfunction develops
Distinguishing from Obesity and Lymphoedema
Pain, tenderness, and easy bruising are intrinsic features of lipedema. Unlike obesity, fat distribution is symmetrical and diet-resistant. Unlike lymphoedema, lipedema is always bilateral with sparing of the feet.
Causes & Risk Factors
- Hormonal triggers: puberty, pregnancy, menopause
- Strong genetic and familial component
- Underrecognised in Asian populations
Treatment Options
- Conservative: medical-grade compression garments, manual lymphatic drainage
- Low-impact exercise and anti-inflammatory diet
- Tumescent or water-assisted liposuction for significant functional impairment
Concerned About Lipedema?
Dr. Peter Chang offers specialist assessment and personalised management at Paragon Medical Centre, Singapore.