From Confusion to Clarity: A 37-Year-Old Woman's Lipedema Story
Dr. Peter Chang
Triple Board-Certified Cardiologist & Vascular Specialist
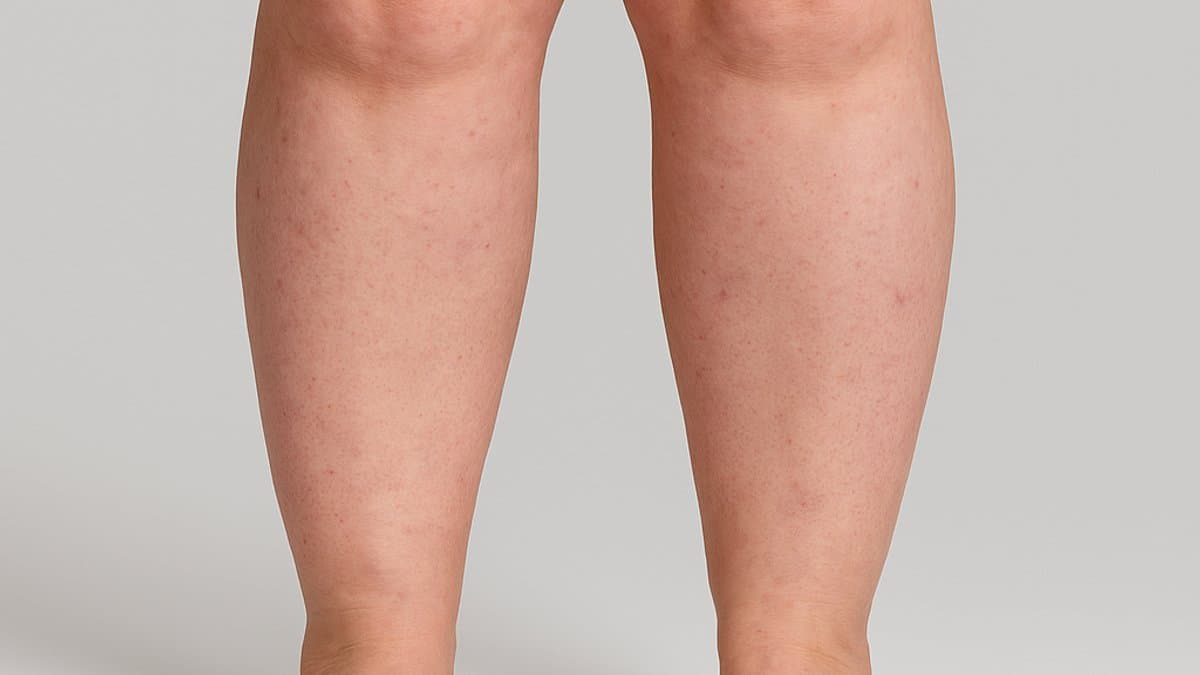
When Her Legs Started Changing
Why Lipedema Is So Difficult to Recognise
Ultrasound: The Imaging That Finally Brought Clarity
- A thickened subcutaneous fat layer with enlarged, nodular fat lobules
- Heterogeneous, grainy tissue pattern
- Thickened fibrous septa that produced pain under compression
- Great saphenous vein valve failure with venous reflux — a second, overlapping diagnosis
Why Venous Reflux Made Everything Worse
Treating the Venous Component First
How She Is Doing Today
Frequently Asked Questions
Common Questions About From Confusion to Clarity
What is the difference between lipedema and lymphedema?
Lipedema is a chronic condition of abnormal fat distribution affecting primarily the legs and sometimes arms, with feet spared. It is painful, causes easy bruising, and does not respond to diet or exercise. Lymphedema is caused by a damaged or underdeveloped lymphatic system and typically involves pitting oedema, skin changes, and can affect one or both limbs including the feet.
Can lipedema be treated without surgery?
Conservative management — medical-grade compression garments, manual lymphatic drainage, anti-inflammatory nutrition, and gentle exercise — can significantly reduce symptoms and slow progression. For those with co-existing venous reflux, treating the vein disease substantially improves conservative treatment outcomes. Lipedema-specific liposuction is considered for advanced cases where conservative management is insufficient.
How is venous reflux diagnosed in Singapore?
Venous reflux is diagnosed with a duplex ultrasound of the lower limb veins — a painless, non-invasive test that maps the anatomy, identifies valve incompetence, and quantifies the degree of reflux. It is essential for any patient with unexplained leg heaviness, swelling, or aching that worsens throughout the day.
Why is it important to treat venous disease before lipedema liposuction?
Untreated venous reflux increases venous pressure in the leg, which worsens swelling and tissue fluid accumulation. Performing liposuction in a limb with active venous hypertension produces worse outcomes and slower healing. Treating the venous disease first normalises the venous environment and leads to significantly better surgical results.